Macular degeneration, also called age-related macular degeneration or AMD, is a common eye condition that affects many people. It is the number one cause of blindness in North America. This progressive eye disease affects the macula in the eye and can cause central vision loss, so it’s important to be aware of your risk for AMD.
Genetics can play a role in a person’s likelihood of developing AMD—having a family history of this condition can increase your risk. However, a family history of AMD doesn’t guarantee that you’ll develop it—genes only play a part in whether or not you may be at risk of developing macular degeneration. Genes may be “switched on or off” based on lifestyle factors. Smoking, UV exposure and diet are the top 3 factors on whether these genes are expressed.
If you’re worried that you or a loved one is at risk of AMD, it’s important to consult your optometrist. Regular eye exams are essential for monitoring the health of your eyes, and with routine exams, we can help diagnose and treat potential eye conditions like AMD in their early stages to help you retain your vision. There is a genetic test that can help determine your risk level to the disease. https://arcticdx.com/
What Is Macular Degeneration?
Macular degeneration, also known as age-related macular degeneration (AMD), is a progressive eye disease that directly affects the central part of your retina. While the exact cause is unknown, it typically involves certain cells in your eyes breaking down or blood vessels leaking small amounts of fluid into the eye, damaging the retina.
This condition usually affects older adults and is one of the leading causes of vision loss.
AMD can be categorized into 2 types:
- Dry macular degeneration, which is significantly more common
- Wet macular degeneration, which is less common but can be more severe
Dry Macular Degeneration
Dry macular degeneration, also known as atrophic AMD, is the more common form of AMD, typically accounting for 90% of cases. When this form begins developing, it often doesn’t have noticeable early symptoms.
In the intermediate stage, this condition begins to progress slowly over time, causing blurry or distorted central vision. It may also cause difficulty seeing in low-light environments.
In the later stages, dry AMD can lead to straight lines appearing wavy, like they’re bent or crooked. It can also cause a blurry or foggy area in your central vision that begins getting larger as AMD continues progressing, leading to difficulty reading or seeing things clearly around you.
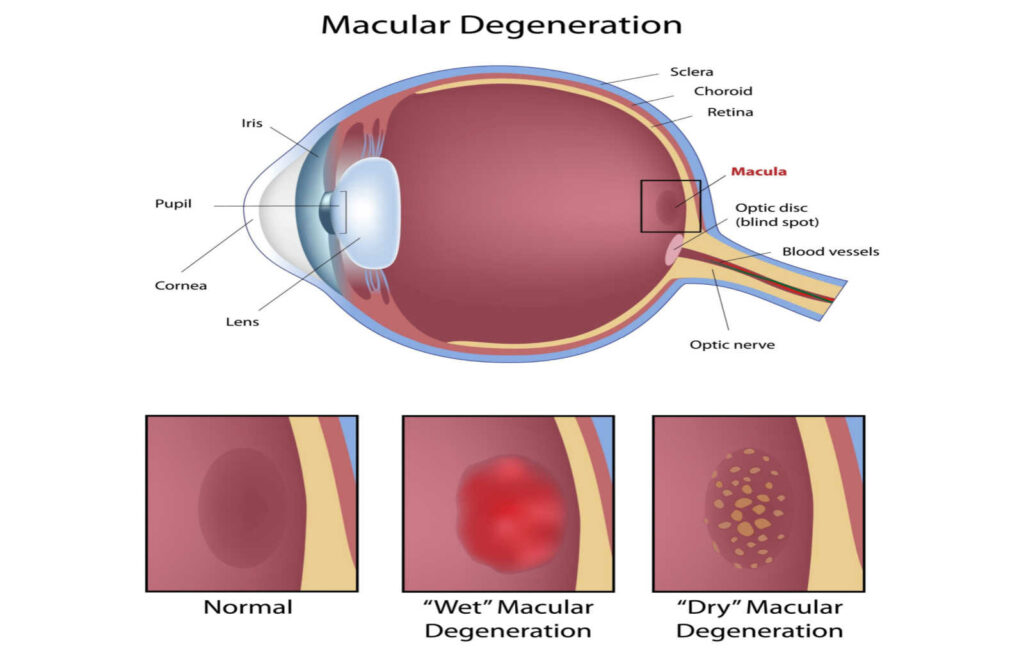
Wet Macular Degeneration
Wet macular degeneration, also known as advanced neovascular AMD, is the significantly less common variant. Wet AMD typically occurs as a result of blood vessels leaking fluids or blood into the eye.
Wet AMD is an eye emergency that can cause a blind spot to develop in the central part of your vision, leading to long-term vision problems. It’s essential to seek prompt emergency eye care for wet AMD.
The Role of Genetics in Macular Degeneration
While the causes of macular degeneration are not fully understood, it is considered a hereditary medical condition—if you have a family history of AMD, you may be more likely to develop the condition yourself. Any increased risk makes it essential to regularly schedule comprehensive eye exams, so an optometrist can determine how healthy your eyes are and your need for future monitoring.
Your genes do play a part in your likelihood of developing this condition, but that doesn’t mean having a certain gene guarantees whether or not you’ll experience macular degeneration in your life. There are also other risk factors and environmental factors to consider.
Your risk of developing AMD can increase if you:
- Smoke
- Are over the age of 50
- Have high blood pressure or high cholesterol
- Eat a diet high in saturated fats
- Have heart disease or cardiovascular problems
- Have had excessive UV exposure
How to Lower Your Risk of Macular Degeneration
Fortunately, several of the AMD risk factors can be controlled. If you’re worried about this condition, it can be extremely beneficial to:
- Quit smoking (or don’t start)
- Exercise and maintain an active lifestyle
- Monitor your blood pressure and cholesterol
- Eat a healthy, nutritious diet
- Wear sunglasses while outdoors
While these habits can’t guarantee that you won’t develop AMD, they can help reduce your potential risk of developing it. If you begin experiencing any changes in your vision, you should visit your optometrist to determine the cause and the recommended treatment.
Support for Macular Degeneration
Your vision is an essential part of your life, so it’s important that you do what you can to keep it clear. This begins with scheduling comprehensive eye exams, so we can monitor any potential changes in your eyes and provide you with the appropriate treatment for conditions like macular degeneration. At See & Be Seen Eyecare, we cherish your vision as much as you do. To speak with a team of caring professionals about your vision, book an appointment with us. We’re here to help you detect, understand, and manage conditions like AMD.